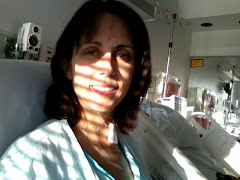
Did not 'graduate' from the tx program on Friday. Somewhat bummed but also wasn't in the right "space" to deal with it on Friday. Besides, "M" wasn't there and the clinic is such a vastly different place without her.
Bloodtests are all dead set normal (except for the platelets which still have to even out) but I need another ultrasound and my drug levels for one of the immunosuppressants are still all wonky.
Sunday, June 28, 2009
Recent Misadventures, Part III
I generally start out procedure days with the Ramones.
Anyone who knows me knows it is no secret that I really, really, really like narcotics. Given a different life, I would be a junkie. In a different era, I would have been one of those ladies taking Laudenum. Morphine and its relatives have a wonderful, pleasant, velveteen mist that descends from the crown of my head and warmly envelopes all of my senses in sunshine. It's a sure-fire way to get that same feeling of utter well being that otherwise takes a perfect day floating on a river, or a just-right bed and the world's best pillow, or the most amazing delicate chocolate torte. You get the picture.
So anyway, when I know that I am going to get fentanyl, I am generally more than okay with the idea. I have had it myriad times over the last ten years or so -- there was a period of about 2 1/2 years during which I was having endoscopic exams every 6 weeks. I have a bit of a tolerance for the stuff. Fentanyl (or demarrol, for those who can take it) is frequently administered with Versed, which is an amnestic. It renders one conscious but completely oblivious.
Put bluntly: fentanyl controls pain, versed enables you to be controlled.
There's a ton of opinion out there about versed, and people who really, really, really hate it. They don't like the idea of not being able to control the situation, not knowing what is going on, not having input on their medical care, etc. I understand the point of view, but I guess it's never bothered me. In fact, it generally results in some really funny stories -- whenever I've had it I've been well in the care of family or friends, so they keep me out of too much trouble... I am very very lucid while on the cocktail, but I don't remember the entire day. It's kind of a nice little holiday from reality in an otherwise straight-laced life.
So when I showed up for my angiogram on May 28 I wasn't worried. I figured I'd be sedated for one or two hours, be out of the outpatient wing by night time, and able to join friends for dinner and games the next night. The clinic was running late, so I made it back an hour late, and spent another hour in prep, hooked up to an iv, and without anything to read and with no iPod to listen to. The prep area is a series of cubbies with curtains, so it's not at all private. I suppose Sarah could have been with me, but I was alone. The family across was waiting for radiology on tumors in the one gentleman's lungs. I gathered from their conversation that the woman's sister (the wife of the other man) had died of cancer. They all were or had been smokers. They were funny and joking in the way of really stressed-out people. There was also a man who was having some sort of procedure to relieve back pain - installation of a pump to deliver painkillers directly, maybe? I shouldn't have been listening... but what else do you do. There were two "codes" while I waited, and one woman who had an allergic reaction to the CT contrast fluid...
So anyway, it's easy to see why they get behind schedule.
The nurse anesthetist came to speak with me about the sedation, and told me what the procedure room would be like (like an operating room... ha ha like I'd ever paid attention inside one of those).
What I didn't expect was so many people. I think there were 5 actual personnel plus maybe 4 more students/interns. The room was big with a glassed off partition with more people and instruments. The angiogram takes place atop an x-ray machine, so everyone in there is operating in lead aprons (I think of their poor knees), which allowed them to guide the catheter to the right place.
I was out cold by the time Dr. V came in. I vaguely recall the soundtrack this day was classic rock, which is cool. (I once had an MRI that was about 1400 years long and it ruined James Taylor for me forever.) There was lots of activity.
Since I wasn't completely unconscious, there are things I do remember from the next -- oh yes -- four hours. Asking for more pain meds at least three times, and then descending back into a pale blue fog.
The only thing I remember about waking up the first time was being told that the procedure had taken about 3 times longer than expected, and they had had to "poke me" an absurd amount of times, each with progressively smaller catheters, because they could not work their way into the portal vein in order to expand the little balloon-type device to expand the vein. I found out not much later that, once there, the vein was blocked nearly 100%.
I also know that I hurt like hell. Not the baseball-sized bruise between my third and fourth ribs, but my entire right torso. I felt like I had been kicked repeatedly by horses, and then flipped around three or four times in a car filled with cannonballs. On the pain scale (1-10) I was fully at an 8. (I hesitate to ever tell that I'm at a 9 or a 10, because I am sure there is always something worse than whatever I might be experiencing at the time.) For me, a really bad charley horse is a 5, and some headaches can get to a 6. Post surgery I hovered in the 4-6 range depending on what I was trying to do.
What was even more pleasant than the pain was that every time I sat up above, say, 45 degrees (let alone walk), I would throw up. Now, considering that I hadn't eaten for - at this point - twenty hours, it was a pretty hideous experience. Not only for me, but for Sarah and Martin, who were hanging out with me. Obviously not going home on Thursday.
Friday rolled around and I hadn't slept and I still hurt terribly. We played "let's give Shirley drugs" all day. Different muscle relaxants, different pain killers (the oxys, atavan, codein, etc.) and still, every time I breathed the pain was excruciating. I think I had another ultrasound that day. I think I remember the nurses were nice. I think Martin was there most of the day, working. I think I was able to eat some clear foods.
The clinic were trying to get someone to admit me to the hospital. I wasn't allowed back to the transplant floor, and there weren't any beds on the correct floor for hepatology. They were also trying to get authorization for a self-administered pain pump for me. Until that time, I was just to wait in the ambulatory out-patient ward. I think Kathy and Gary came to visit and have dinner with Martin.
Saturday morning came. My parents were there with Marcie. I refused the pain pump and just begged them to let me go home.
The weird thing was that the dr. that was responsible for me (Dr. V) was at another hospital doing procedures all day, so getting discharge authorization took some work. The hitch was that if I needed pain meds he couldn't prescribe them since a real signature was necessary. I explained in what I thought were very polite tones, given the situation, that I had a whole bottle of painkillers at home so please couldn't they let me leave!
And I was out by 1. Thank the gods. With a new prescription for Plavix (yum) and still at a pain level 7. I could. Not. Breathe.
Anyone who knows me knows it is no secret that I really, really, really like narcotics. Given a different life, I would be a junkie. In a different era, I would have been one of those ladies taking Laudenum. Morphine and its relatives have a wonderful, pleasant, velveteen mist that descends from the crown of my head and warmly envelopes all of my senses in sunshine. It's a sure-fire way to get that same feeling of utter well being that otherwise takes a perfect day floating on a river, or a just-right bed and the world's best pillow, or the most amazing delicate chocolate torte. You get the picture.
So anyway, when I know that I am going to get fentanyl, I am generally more than okay with the idea. I have had it myriad times over the last ten years or so -- there was a period of about 2 1/2 years during which I was having endoscopic exams every 6 weeks. I have a bit of a tolerance for the stuff. Fentanyl (or demarrol, for those who can take it) is frequently administered with Versed, which is an amnestic. It renders one conscious but completely oblivious.
Put bluntly: fentanyl controls pain, versed enables you to be controlled.
There's a ton of opinion out there about versed, and people who really, really, really hate it. They don't like the idea of not being able to control the situation, not knowing what is going on, not having input on their medical care, etc. I understand the point of view, but I guess it's never bothered me. In fact, it generally results in some really funny stories -- whenever I've had it I've been well in the care of family or friends, so they keep me out of too much trouble... I am very very lucid while on the cocktail, but I don't remember the entire day. It's kind of a nice little holiday from reality in an otherwise straight-laced life.
So when I showed up for my angiogram on May 28 I wasn't worried. I figured I'd be sedated for one or two hours, be out of the outpatient wing by night time, and able to join friends for dinner and games the next night. The clinic was running late, so I made it back an hour late, and spent another hour in prep, hooked up to an iv, and without anything to read and with no iPod to listen to. The prep area is a series of cubbies with curtains, so it's not at all private. I suppose Sarah could have been with me, but I was alone. The family across was waiting for radiology on tumors in the one gentleman's lungs. I gathered from their conversation that the woman's sister (the wife of the other man) had died of cancer. They all were or had been smokers. They were funny and joking in the way of really stressed-out people. There was also a man who was having some sort of procedure to relieve back pain - installation of a pump to deliver painkillers directly, maybe? I shouldn't have been listening... but what else do you do. There were two "codes" while I waited, and one woman who had an allergic reaction to the CT contrast fluid...
So anyway, it's easy to see why they get behind schedule.
The nurse anesthetist came to speak with me about the sedation, and told me what the procedure room would be like (like an operating room... ha ha like I'd ever paid attention inside one of those).
What I didn't expect was so many people. I think there were 5 actual personnel plus maybe 4 more students/interns. The room was big with a glassed off partition with more people and instruments. The angiogram takes place atop an x-ray machine, so everyone in there is operating in lead aprons (I think of their poor knees), which allowed them to guide the catheter to the right place.
I was out cold by the time Dr. V came in. I vaguely recall the soundtrack this day was classic rock, which is cool. (I once had an MRI that was about 1400 years long and it ruined James Taylor for me forever.) There was lots of activity.
Since I wasn't completely unconscious, there are things I do remember from the next -- oh yes -- four hours. Asking for more pain meds at least three times, and then descending back into a pale blue fog.
The only thing I remember about waking up the first time was being told that the procedure had taken about 3 times longer than expected, and they had had to "poke me" an absurd amount of times, each with progressively smaller catheters, because they could not work their way into the portal vein in order to expand the little balloon-type device to expand the vein. I found out not much later that, once there, the vein was blocked nearly 100%.
I also know that I hurt like hell. Not the baseball-sized bruise between my third and fourth ribs, but my entire right torso. I felt like I had been kicked repeatedly by horses, and then flipped around three or four times in a car filled with cannonballs. On the pain scale (1-10) I was fully at an 8. (I hesitate to ever tell that I'm at a 9 or a 10, because I am sure there is always something worse than whatever I might be experiencing at the time.) For me, a really bad charley horse is a 5, and some headaches can get to a 6. Post surgery I hovered in the 4-6 range depending on what I was trying to do.
What was even more pleasant than the pain was that every time I sat up above, say, 45 degrees (let alone walk), I would throw up. Now, considering that I hadn't eaten for - at this point - twenty hours, it was a pretty hideous experience. Not only for me, but for Sarah and Martin, who were hanging out with me. Obviously not going home on Thursday.
Friday rolled around and I hadn't slept and I still hurt terribly. We played "let's give Shirley drugs" all day. Different muscle relaxants, different pain killers (the oxys, atavan, codein, etc.) and still, every time I breathed the pain was excruciating. I think I had another ultrasound that day. I think I remember the nurses were nice. I think Martin was there most of the day, working. I think I was able to eat some clear foods.
The clinic were trying to get someone to admit me to the hospital. I wasn't allowed back to the transplant floor, and there weren't any beds on the correct floor for hepatology. They were also trying to get authorization for a self-administered pain pump for me. Until that time, I was just to wait in the ambulatory out-patient ward. I think Kathy and Gary came to visit and have dinner with Martin.
Saturday morning came. My parents were there with Marcie. I refused the pain pump and just begged them to let me go home.
The weird thing was that the dr. that was responsible for me (Dr. V) was at another hospital doing procedures all day, so getting discharge authorization took some work. The hitch was that if I needed pain meds he couldn't prescribe them since a real signature was necessary. I explained in what I thought were very polite tones, given the situation, that I had a whole bottle of painkillers at home so please couldn't they let me leave!
And I was out by 1. Thank the gods. With a new prescription for Plavix (yum) and still at a pain level 7. I could. Not. Breathe.
Thursday, June 11, 2009
Recent Misadventures, Part II
May 22 started at oh-dark-thirty, as usual, for the 6:30 blood draw. Fasting, you know, since I was scheduled for sedation at 10, and involving the patented Schultz family transportation nightmare. To wit: Marcie leaving Kitsap at dawn to pick me up to go get Sarah since Sarah doesn't have a car to go to the UW where Marcie will meet Neal who has his car so the two of them can roadtrip to Wyoming and Sarah can drive me home and stay with me and have the car for the week.
Phew.
Me: coffee-less. Stomach growly, with the two of them in the radiology waiting room. This room is slightly larger than my bed. (Not my bedroom, my bed.) And serves as the waiting room for about 400 different clinics. And people in there are not happy people -- mostly sleep deprived and food deprived, and worried. There are moms-to-be waiting for ultrasounds, people waiting for angiography, people waiting for MRI's and CT scans to tell them all sorts of scary things about what's in their body, and a tank of really forlorn fish.
The staff, however, are terrific. I have been there a LOT. I know. They are always friendly and efficient, and generally they operate on time. The only time I have had a bad time in radiology has been when I've been horribly ill (or recently surgeoned); and then it's all because of me. :-)
Anyhow, I was early, as always. When I've had CT's or ultrasounds, I have found that if I show up early, sometimes I can be seen early. So on this particular morning, we were in the waiting room by 9, and checked in, and waiting in what I wish was a quiet manner, but... well, that's hard for me and anyone from my corner of the genetic pool.
At about 9:15, a very nice lady in scrubs, hair cover, and raised mask joins the three of us in the waiting room, and -- all seats being occupied -- perches herself on the (tippy) occasional table, atop a pile of sudoku and crayons. She asks "I want to know what you think you are here for today."
This is not the question I was expecting. But I answered it anyhow: I think I am here for an angiogram, with possible angioplasty and a stent. EEEENNH. No points for me. The nice nurse points out that no, this is not a simple procedure and I need to have a clinic appointment with the dr. first to go over the procedure, risks, options, etc. Only today is not a clinic day and he is in a procedure, but since I am scheduled for the 10 a.m. time he can see me in his office.
?????
Now, I have no qualms about a dr. wanting to see me before he sticks large needles and catheters into my liver, but I have put my trust in the scheduling gods in the tx clinic, and have assumed that they communicate with other dr.s who will be doing procedures. Maybe they do. Maybe they don't. In this case, I was actually really pleased that the dr. was willing to be flexible to do an office visit on a procedures day, and to go through the process with me.
Plus I got the chance to get coffee and breakfast before meeting with him.
By 10:30 (they do run late, after all) Sarah and I were being escorted into the small windowless office in a bank of physician offices. Do these people get any benefits? I think it would be possible to be a staff member at that hospital and, during NW winters, not see the sun for months at a time. But I digress.
Dr. V was not what I expected. Let's just say that he has a name which would imply a particular ethnicity and a personage which belies that name. But after that initial "huh" moment, he is a nice nice gentleman. For instance, this is the first time that a dr. has brought up images of a CT or any other imagery of my myriad tests. I think it's just my failure to ask (they are all electronic and available to any dr.) but it was nice to have that as a starting point.
An aside: my new liver is smooth, and happy looking. Like the pictures you see in text books. I haven't yet seen a picture of my old liver; I will have to ask about that.
Dr. V explained the method for a percutaneous transhepatic angiogram -- which basically means they go through my skin right into my liver, and cross the liver till they get to the portal vein. There would be some pain - but not as much as possible because, well, I don't have any nerve endings in my new liver. I still do in the rest of my body, though! The dr. explained the possibilities of what could/would happen once inside - that the first attempt would be angioplasty (i.e., insertion of little balloons, then inflation) to clear the blockage in my vein. He discussed the possibility of a stent, which was later ix-nayed by Dr. H. He talked about the sedation and the effects of sedation (with which I am well accustomed). Then he handed me the patient release.
I think this is where I got myself in trouble. I actually read the release... Yeah, I know, I should have been reading all the fine print before, but skimming always proved that I had already received all the information verbally.
One clause elicited a "huh" from me: the statement that, due to the maneuvering of the catheter within my body, or due to the position in which my body would be placed during the procedure, it was possible that I would experience additional pain, like back pain. I allowed as to how every time I'd had procedures before, I had had residual pain in my upper back and sometimes shoulder, and that no doctor had ever really believed me... so I felt a little vindicated that this was actually stated with the angiography.
We arranged for an appointment the following Thursday, May 28.
Sarah and I played hooky the rest of the day, and it was an unexpected day, and it was fun. When the sun shines here it is so glorious, and when you have a borrowed little red car and a gracious niece, the world is good.
Phew.
Me: coffee-less. Stomach growly, with the two of them in the radiology waiting room. This room is slightly larger than my bed. (Not my bedroom, my bed.) And serves as the waiting room for about 400 different clinics. And people in there are not happy people -- mostly sleep deprived and food deprived, and worried. There are moms-to-be waiting for ultrasounds, people waiting for angiography, people waiting for MRI's and CT scans to tell them all sorts of scary things about what's in their body, and a tank of really forlorn fish.
The staff, however, are terrific. I have been there a LOT. I know. They are always friendly and efficient, and generally they operate on time. The only time I have had a bad time in radiology has been when I've been horribly ill (or recently surgeoned); and then it's all because of me. :-)
Anyhow, I was early, as always. When I've had CT's or ultrasounds, I have found that if I show up early, sometimes I can be seen early. So on this particular morning, we were in the waiting room by 9, and checked in, and waiting in what I wish was a quiet manner, but... well, that's hard for me and anyone from my corner of the genetic pool.
At about 9:15, a very nice lady in scrubs, hair cover, and raised mask joins the three of us in the waiting room, and -- all seats being occupied -- perches herself on the (tippy) occasional table, atop a pile of sudoku and crayons. She asks "I want to know what you think you are here for today."
This is not the question I was expecting. But I answered it anyhow: I think I am here for an angiogram, with possible angioplasty and a stent. EEEENNH. No points for me. The nice nurse points out that no, this is not a simple procedure and I need to have a clinic appointment with the dr. first to go over the procedure, risks, options, etc. Only today is not a clinic day and he is in a procedure, but since I am scheduled for the 10 a.m. time he can see me in his office.
?????
Now, I have no qualms about a dr. wanting to see me before he sticks large needles and catheters into my liver, but I have put my trust in the scheduling gods in the tx clinic, and have assumed that they communicate with other dr.s who will be doing procedures. Maybe they do. Maybe they don't. In this case, I was actually really pleased that the dr. was willing to be flexible to do an office visit on a procedures day, and to go through the process with me.
Plus I got the chance to get coffee and breakfast before meeting with him.
By 10:30 (they do run late, after all) Sarah and I were being escorted into the small windowless office in a bank of physician offices. Do these people get any benefits? I think it would be possible to be a staff member at that hospital and, during NW winters, not see the sun for months at a time. But I digress.
Dr. V was not what I expected. Let's just say that he has a name which would imply a particular ethnicity and a personage which belies that name. But after that initial "huh" moment, he is a nice nice gentleman. For instance, this is the first time that a dr. has brought up images of a CT or any other imagery of my myriad tests. I think it's just my failure to ask (they are all electronic and available to any dr.) but it was nice to have that as a starting point.
An aside: my new liver is smooth, and happy looking. Like the pictures you see in text books. I haven't yet seen a picture of my old liver; I will have to ask about that.
Dr. V explained the method for a percutaneous transhepatic angiogram -- which basically means they go through my skin right into my liver, and cross the liver till they get to the portal vein. There would be some pain - but not as much as possible because, well, I don't have any nerve endings in my new liver. I still do in the rest of my body, though! The dr. explained the possibilities of what could/would happen once inside - that the first attempt would be angioplasty (i.e., insertion of little balloons, then inflation) to clear the blockage in my vein. He discussed the possibility of a stent, which was later ix-nayed by Dr. H. He talked about the sedation and the effects of sedation (with which I am well accustomed). Then he handed me the patient release.
I think this is where I got myself in trouble. I actually read the release... Yeah, I know, I should have been reading all the fine print before, but skimming always proved that I had already received all the information verbally.
One clause elicited a "huh" from me: the statement that, due to the maneuvering of the catheter within my body, or due to the position in which my body would be placed during the procedure, it was possible that I would experience additional pain, like back pain. I allowed as to how every time I'd had procedures before, I had had residual pain in my upper back and sometimes shoulder, and that no doctor had ever really believed me... so I felt a little vindicated that this was actually stated with the angiography.
We arranged for an appointment the following Thursday, May 28.
Sarah and I played hooky the rest of the day, and it was an unexpected day, and it was fun. When the sun shines here it is so glorious, and when you have a borrowed little red car and a gracious niece, the world is good.
Sunday, June 7, 2009
Recent Misadventures, Part I
I think the last time I posted a legitimate update I wrote about "oh crap, I need an angiogram." I was scheduled for May 22 and was not looking forward to it, only it didn't happen that day...
Okay, let me start from the beginning, and 'splain what it is that the portal vein does. Apologies for my tenuous grasp on anatomy... but if you want totally specific information you'll have to do your research.
ANYWAY, it's a little-known fact that the liver exists almost entirely on dirty blood. That is, about 80% of the liver's blood supply comes from the stomach and the small intestine, after those two organs have done their peristaltic and enzymatic magic and imbued the blood with all sorts of raw materials for living. The liver then takes that dirty blood and not only takes care of itself but also takes those materials and refines them into useable stuff for the body -- proteins, sugars -- and processes out the waste matter. This chemical cooker also creates heat and energy for the body to use.
Well, that 80% of the blood travels through one key vessel: the portal vein. This vein is about 8 centimeters long and one centimeter in diameter and is located roughly at the level of the bottom of a bra strap (only on the other side of the spinal column). It consists of the junction of two major veins which in turn drain all of the abdominal organs. The lienal vein brings in blood from the stomach, pancreas, and the descending and lower parts of the intestinal system via the spleen -- if I had a spleen -- but those have been rerouted for the direct connection. The mesenteric vein, roughly to the left/lower portion of the whole intersection, brings in blood from the middle parts of the digestive system, all the ascending and transverse parts, and parts of the stomach.
So it's kind of a big deal.
When I got my new liver, my old vein was hooked to the new vein at about the 4-centimeter mark. There was a blood clot there that took some time to remove in surgery, and then there were sutures there (are they called sutures when they're inside?) to connect my old portal vein to the new one. The two were/are probably close to the same size, but since the portal vein is often messy when there's been long-term cirrhosis, the old and new ends may have been different.
Portal vein hypertension -- that is, too much blood pressure in the portal vein -- is also a big deal. It's one of the effects/indicators of liver disease. Basically that portal vein gets blocked, scarred, or otherwise mucked up so that the blood cannot get into the liver. Therefore it tends to back up... and then take the path of least resistance. Blood that backs up into the vein through the stomach pushes its way out through the capillaries in the stomach or esophogus walls, causing varices. Those are varicose veins in the stomach/esophogeal lining which can burst without notice and cause a person to bleed to death. I had been taking blood pressure meds to prevent such bleeds for about the last 5 years. Portal vein hypertension can also cause bleeding in other parts of the intestinal tract, can render the body inable to rid itself of fluids (resulting in the round, hard stomach), and can cause a pattern of varicose veins on the lower abdomen. I have had the pleasure of experiencing all of the above (not so bad with the abdomen veins, though).
So when I had the routine ultrasound to look at blood flow in my liver, and the follow-up CT, both of which showed that the portal vein was narrowed, it needed to be fixed. As Dr. H said it: 'we expect you to have this liver for a long time and we want it to function perfectly' and thus I was scheduled to meet with Dr. V, the Inteventional Radiologist, for the angiogram...
Okay, let me start from the beginning, and 'splain what it is that the portal vein does. Apologies for my tenuous grasp on anatomy... but if you want totally specific information you'll have to do your research.
ANYWAY, it's a little-known fact that the liver exists almost entirely on dirty blood. That is, about 80% of the liver's blood supply comes from the stomach and the small intestine, after those two organs have done their peristaltic and enzymatic magic and imbued the blood with all sorts of raw materials for living. The liver then takes that dirty blood and not only takes care of itself but also takes those materials and refines them into useable stuff for the body -- proteins, sugars -- and processes out the waste matter. This chemical cooker also creates heat and energy for the body to use.
Well, that 80% of the blood travels through one key vessel: the portal vein. This vein is about 8 centimeters long and one centimeter in diameter and is located roughly at the level of the bottom of a bra strap (only on the other side of the spinal column). It consists of the junction of two major veins which in turn drain all of the abdominal organs. The lienal vein brings in blood from the stomach, pancreas, and the descending and lower parts of the intestinal system via the spleen -- if I had a spleen -- but those have been rerouted for the direct connection. The mesenteric vein, roughly to the left/lower portion of the whole intersection, brings in blood from the middle parts of the digestive system, all the ascending and transverse parts, and parts of the stomach.
So it's kind of a big deal.
When I got my new liver, my old vein was hooked to the new vein at about the 4-centimeter mark. There was a blood clot there that took some time to remove in surgery, and then there were sutures there (are they called sutures when they're inside?) to connect my old portal vein to the new one. The two were/are probably close to the same size, but since the portal vein is often messy when there's been long-term cirrhosis, the old and new ends may have been different.
Portal vein hypertension -- that is, too much blood pressure in the portal vein -- is also a big deal. It's one of the effects/indicators of liver disease. Basically that portal vein gets blocked, scarred, or otherwise mucked up so that the blood cannot get into the liver. Therefore it tends to back up... and then take the path of least resistance. Blood that backs up into the vein through the stomach pushes its way out through the capillaries in the stomach or esophogus walls, causing varices. Those are varicose veins in the stomach/esophogeal lining which can burst without notice and cause a person to bleed to death. I had been taking blood pressure meds to prevent such bleeds for about the last 5 years. Portal vein hypertension can also cause bleeding in other parts of the intestinal tract, can render the body inable to rid itself of fluids (resulting in the round, hard stomach), and can cause a pattern of varicose veins on the lower abdomen. I have had the pleasure of experiencing all of the above (not so bad with the abdomen veins, though).
So when I had the routine ultrasound to look at blood flow in my liver, and the follow-up CT, both of which showed that the portal vein was narrowed, it needed to be fixed. As Dr. H said it: 'we expect you to have this liver for a long time and we want it to function perfectly' and thus I was scheduled to meet with Dr. V, the Inteventional Radiologist, for the angiogram...
Monday, June 1, 2009
06.01.09
Must write. Much to write about.
First must surpass block -- writing actual real letter to donor family.
Then will 'blog.
Will be awhile.
First must surpass block -- writing actual real letter to donor family.
Then will 'blog.
Will be awhile.
Subscribe to:
Comments (Atom)